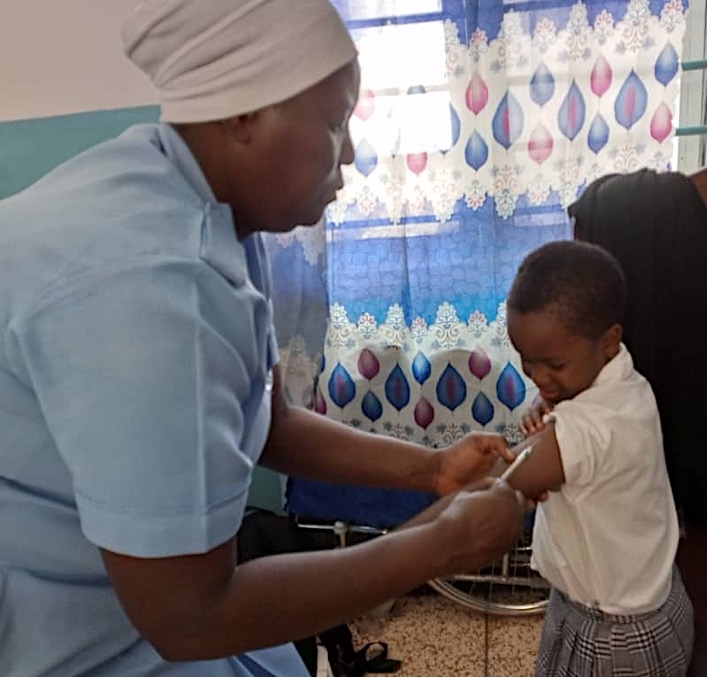
A new study has revealed that expanding access to life-saving rabies vaccines through improved delivery systems and adopting dose-saving methods could significantly reduce deaths in underserved areas of Kenya and Tanzania.
Published in the journal Vaccine, the study—conducted by researchers from the University of Glasgow, Ifakara Health Institute, University of Nairobi’s Centre for Epidemiological Modelling and Analysis (CEMA), University of Edinburgh, and Washington State University—shows that using the World Health Organization’s (WHO) intradermal (ID) method of administering rabies vaccines can reduce vaccine use by over 55 percent, while increasing access in remote areas.
The research emphasizes that rabies, though nearly 100 percent preventable with timely post-exposure prophylaxis (PEP), still kills approximately 59,000 people globally each year—most of them in low- and middle-income countries where access to vaccines is limited.
“It is unacceptable that people are still dying from rabies when effective vaccines are available,” said Martha Luka, lead author and postgraduate researcher at the University of Glasgow. “By improving stock management and adopting dose-sparing intradermal vaccination, countries can protect more people with fewer resources.”
In Kenya and Tanzania, where rabies deaths are still common, access to PEP is often limited by high costs, frequent stockouts, and long travel distances to central hospitals. The new study addresses these barriers through data-driven modelling that evaluates supply chain efficiency, vaccine demand, and facility-level restocking strategies.
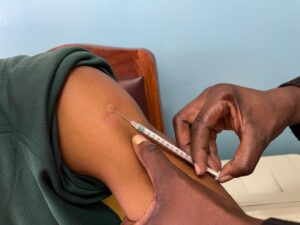
Kennedy Lushasi, co-author and researcher at Ifakara Health Institute, stressed the importance of decentralization: “In Tanzania, where PEP is usually limited to central hospitals, making it available in more local clinics can drastically improve access and equity.”
The research team developed simple, context-specific guidelines to help health facilities determine how much vaccine to stock and when to reorder. These recommendations are designed to help health systems respond quickly to demand spikes and avoid life-threatening shortages.
The findings come at a pivotal time as Gavi, the Vaccine Alliance, begins funding expanded access to rabies vaccines in Africa, Asia, and other regions. The global goal—known as “Zero by 30”—aims to eliminate human deaths from dog-mediated rabies by 2030.
“Gavi’s investment is a transformative milestone,” said Mumbua Mutunga, a co-author and PhD Fellow at CEMA, University of Nairobi. “Our research shows that with the right strategies, including intradermal vaccination and integrated supply chains, we can deliver sustainable protection even in hard-to-reach areas.”
The study also highlighted the need for dog vaccinations, since dogs are the main source of rabies infections in humans. Effective rabies control must include both human PEP and dog immunization efforts.
The researchers are calling on policymakers in Kenya, Tanzania, and beyond to act on the evidence. “Every life lost to rabies is a tragedy—one we now have the tools to prevent,” said Lushasi. “By integrating vaccines into routine systems and reaching more people in rural areas, we can save lives and build more resilient health systems.”
Luka added, “With the right strategies in place, achieving zero rabies deaths by 2030 is entirely possible. Now is the time for countries to leverage Gavi’s investment and build stronger, more equitable health systems.”