By Waihiga K. Muturi, Rtn
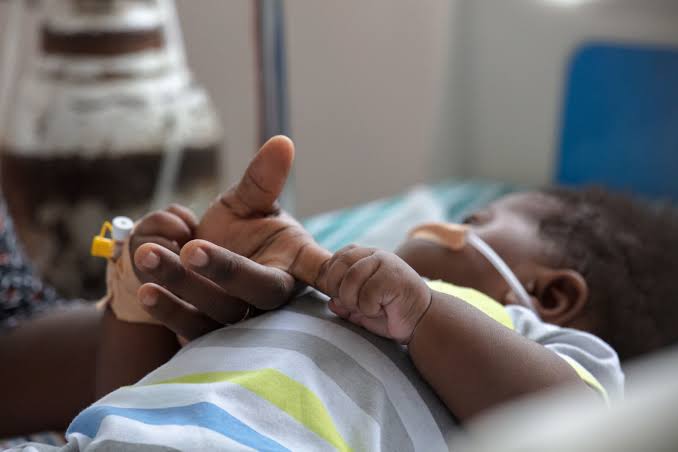
Mama Baraka lost her 4-year-old son in 2024, and her world came crashing down. Her uploads on TikTok detail the young family’s painful journey trying to save their baby boy’s life as he ailed in the hospital, to trying to recover from his eventual, unfortunate death.
Baby Brylejones Baraka died after a prolonged health struggle involving a liver transplant, sepsis, and ultimately, multiple organ failure due to undiagnosed malignant tumours. Her story has touched many, with over 520,000 views and an outpouring of condolences.
According to the mother, Baraka was born with health issues. They were discharged and returned home, but at 5 weeks, they went back to the hospital. Eventually, the baby’s health worsened to the point that he became malnourished at 6 months, and on his first birthday, they were advised to consider a transplant because his liver was deteriorating rapidly.
“Baby Baraka was a post-liver transplant; he was on immunosuppressive medication. He had sepsis, acute infection, for which we got admitted for three weeks, and there was no change,” she shares tearfully in a July 2024 post.
A recent study by the Child Health and Mortality Prevention Surveillance (CHAMPS) Network, in collaboration with the Kenya Medical Research Institute (KEMRI), revealed that 86.9 percent of childhood deaths in high-mortality settings are linked to infections. Even more startling, over 82 percent of these deaths were deemed preventable by expert panels.
Dr. Victor Akelo, Senior Director at CHAMPS and a lead researcher at KEMRI, explains that while child mortality had been on a declining trend before 2015, the progress was not commensurate with the resources being invested. This prompted a deeper inquiry into the true causes of under-five deaths.
“CHAMPS was established to explore these deaths using a more culturally sensitive method—Minimally Invasive Tissue Sampling (MITS),” says Dr. Akelo. This technique, which involves extracting tissue samples using special needles, offers a less intrusive alternative to full autopsies and has proven effective in identifying the exact causes of death.
The cross-sectional study analyzed 632 deaths of children aged 1–59 months from sites across Africa and South Asia, including Kisumu and Siaya counties in Kenya. The most common culprits: malnutrition, HIV, malaria, respiratory infections, and diarrheal diseases.
Alarmingly, the study also found that many infections, particularly those caused by Klebsiella pneumoniae and Acinetobacter baumannii, were hospital-acquired. These findings highlight the urgent need to strengthen infection control in healthcare facilities.
“If surfaces aren’t disinfected, if tools aren’t sterilized, these pathogens can spread easily, just like we saw during COVID-19,” warns Dr. Akelo. He emphasizes that improving infection prevention protocols can significantly reduce child deaths.
Paediatricians on the frontline echo these concerns. Dr. Isaac Kihurani of Aga Khan University Hospital says that even with the best efforts, preventable deaths still happen, and they leave lasting emotional impacts on caregivers and medical staff.
Dr. Aura Nzinga adds that when a child dies from something preventable, the entire paediatric team undergoes debriefs to assess where systemic errors may have occurred and how care can be improved.
Infections aren’t the only concern. For diseases like HIV, prevention of mother-to-child transmission remains a top priority. Health experts stress early detection, proper maternal care, and psychological support for children living with HIV.
With evidence in hand, researchers and doctors are urging governments …
to act decisively. CHAMPS has provided a roadmap. What remains is political will, funding, and swift policy implementation—especially in rural and underserved areas.
The case of young Baraka is heartbreaking, but his story sheds light on a much larger, solvable crisis. If action is taken now, the tragic deaths of children under five can become a rarity rather than the norm.